Are you a US healthcare professional?
INDICATION
RYTELO® (imetelstat) is indicated for the treatment of adult patients with low- to intermediate-1 risk myelodysplastic syndromes (MDS) with transfusion-dependent anemia requiring 4 or more red blood cell units over 8 weeks who have not responded to or have lost response to or are ineligible for erythropoiesis-stimulating agents (ESA). See more
In second-line LR-MDS, give your eligible patients
The possibility of zero
transfusions1

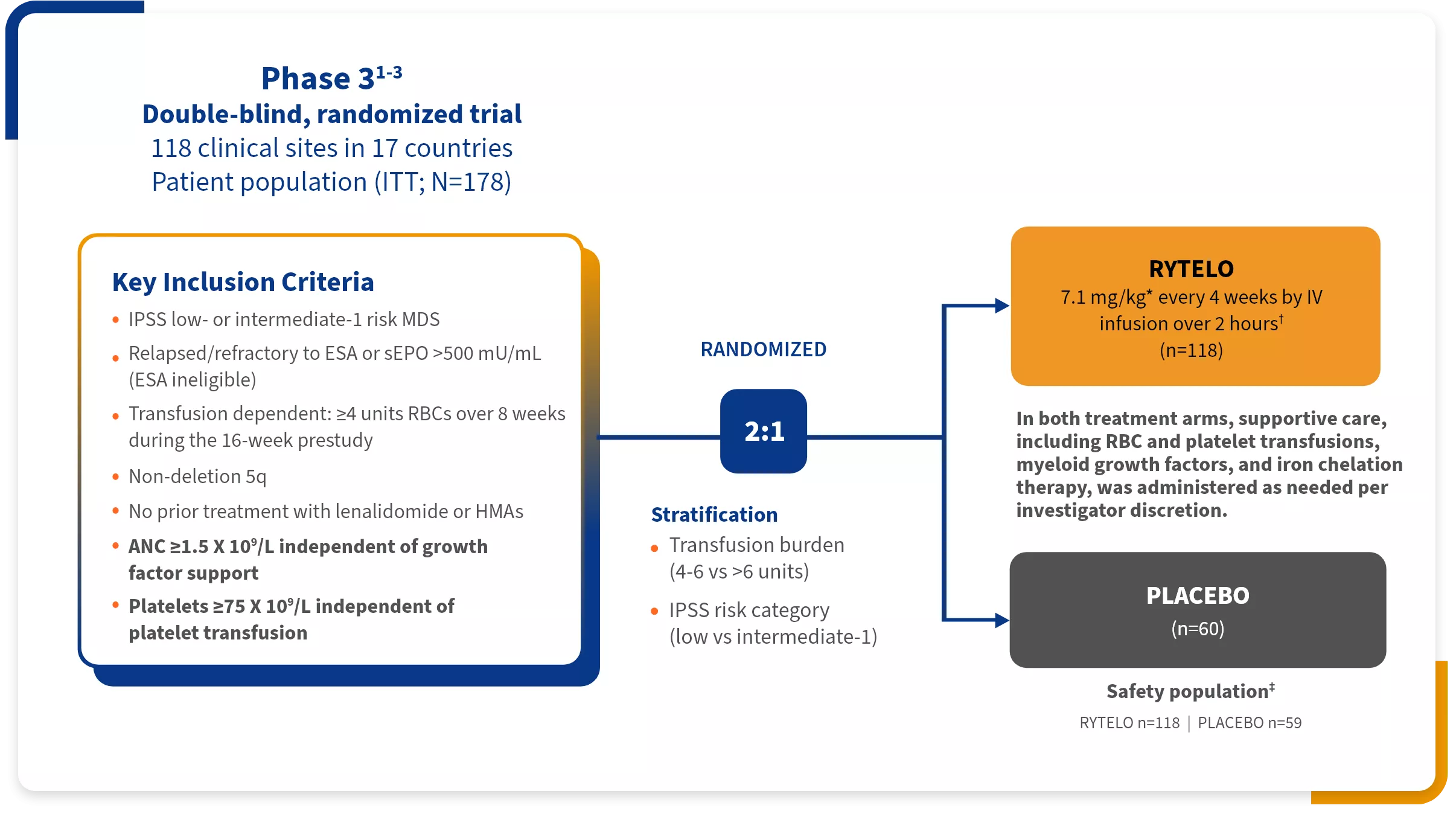
Study design: IMerge was a phase 3, double-blind, placebo-controlled clinical trial evaluating patients with ESA-relapsed, ESA-refractory, or ESA-ineligible LR-MDS (low or intermediate-1 as per IPSS criteria). Prior to randomization, patients required ≥4 units over an 8-week period. Patients had not received prior treatment with either an HMA or lenalidomide and were non-del(5q). Supportive care, including RBC and platelet transfusions, myeloid growth factors, and iron chelation therapy, was administered as needed per investigator discretion.1,2
RYTELO was studied in the IMerge phase 3 clinical trial1
View content
The IMerge phase 3 clinical trial assessed the safety and efficacy of RYTELO (n=118) vs placebo (n=60) in LR-MDS patients with transfusion-dependent anemia1

Primary Endpoint
- ≥8 consecutive weeks of RBC-TI§
Key Secondary Endpoints
- ≥24 consecutive weeks of RBC-TI||
- Time to and duration of RBC-TI in patients who achieved ≥8-week RBC-TI
- Rate of hematologic improvement–erythroid, measured by Hgb increase or RBC transfusion unit reduction (HI-E per IWG 2006)
The approved 7.1 mg/kg dose of imetelstat (active moiety) equates to 7.5 mg/kg imetelstat sodium (the salt) referenced in trial publications.
Patients were pretreated with diphenhydramine and hydrocortisone, or equivalents, prior to dosing.
The safety analysis set included all patients who received at least 1 dose of study drug.
8-week RBC-TI, defined as the proportion of patients without RBC transfusions for ≥8 consecutive weeks starting on the day of randomization until subsequent anticancer therapy, if any.
24-week RBC-TI, defined as the proportion of patients without RBC transfusions for ≥24 consecutive weeks starting on the day of randomization until subsequent anticancer therapy, if any.
The IMerge trial represented a wide spectrum of LR-MDS patients1
ESA-relapsed


RS+ includes: refractory anemia with RS/refractory cytopenia with multilineage dysplasia and ≥15% RS.
RS- includes: others.
Prior RBC transfusion burden is defined as the maximum number of RBC units transfused over an 8-week period during the 16 weeks prior to randomization.
RYTELO provided continuous RBC transfusion independence vs placebo, including for RS- patients1



▼Limitations: These analyses were prespecified, descriptive in nature, did not control for type 1 error, and should be interpreted with caution.
Adapted from Platzbecker U and Santini V, et al. Lancet. 2024.
††Kaplan-Meier estimates of duration of RBC-TI; 8-week TI responder analysis set; HR is from the Cox proportional hazard model, stratified by prior RBC transfusion burden (≤6 vs >6 units RBC) and IPSS risk group (low vs intermediate-1), with treatment as the only covariate.2
RYTELO: Hgb increase and mDoR

▼Limitations: This analysis was prespecified, descriptive in nature, did not control for type 1 error, and should be interpreted with caution.

▼Limitations: This analysis was prespecified, descriptive in nature, did not control for type 1 error, and should be interpreted with caution.



■Limitations: These post hoc analyses were descriptive in nature, not prespecified, and did not control for type 1 error. Interpret with caution as results could represent chance findings.

Subgroup analyses of ≥8-week RBC-TI responders1,6


▼Limitations: These subgroup analyses were prespecified, descriptive in nature, and did not control for type 1 error.
Interpret with caution as results could represent chance findings.
Adapted from Platzbecker U and Santini V, et al. Lancet. 2024.
‡‡CI is provided for descriptive purposes only.
§§One patient in the RYTELO arm was missing the RS category.
¶¶Missing data for 5 patients in RYTELO arm and 2 patients in placebo arm for the sEPO at baseline category.
ANC, absolute neutrophil count; ESA, erythropoiesis; Hgb, hemoglobin; HI-E, hematologic improvement–erythroid; HMA, hypomethylating agent; HR, hazard ratio; IPSS, International Prognostic Scoring System; ITT, intent to treat; IV, intravenous; IWG, International Working Group; LR-MDS, lower-risk myelodysplastic syndromes; mDoR, median duration of response; MDS, myelodysplastic syndromes; NE, not estimable; RBC, red blood cell; RBC-TI, red blood cell transfusion independence; RS, ring sideroblasts; sEPO, serum erythropoietin; TI, transfusion independent; WHO, World Health Organization.
References: 1. RYTELO. Prescribing information. Geron Corp.; 2024. 2. Platzbecker U and Santini V, et al. Imetelstat in patients with lower-risk myelodysplastic syndromes who have relapsed or are refractory to erythropoiesis-stimulating agents (IMerge): a multinational, randomised, double-blind, placebo-controlled, phase 3 trial. Lancet. 2024;403(10423):249-260. 3. Data on file. Geron Corporation. Foster City, CA. 4. Zeidan AM, Santini V, Platzbecker U, et al. Efficacy of imetelstat on red blood cell (RBC)-transfusion independence (TI) in the absence of platelet transfusions or myeloid growth factors in IMerge. J Clin Oncol. 2024;42(suppl16):6566. 5. Platzbecker U, Komrokji RS, Zeidan AM, et al. Durable continuous transfusion independence with imetelstat in IMerge phase 3 for patients with heavily transfused non-del(5q) lower-risk myelodysplastic syndromes relapsed/refractory to or ineligible for erythropoiesis-stimulating agents. Blood. 2023;142(suppl 1):4605. 6. Platzbecker U and Santini V, et al. Imetelstat in patients with lower-risk myelodysplastic syndromes who have relapsed or are refractory to erythropoiesis stimulating agents (IMerge): a multinational, randomised, double-blind, placebo-controlled, phase 3 trial. Lancet. 2024;(suppl)403(10423):published online Dec 1.
INDICATION
RYTELO® (imetelstat) is indicated for the treatment of adult patients with low- to intermediate-1 risk myelodysplastic syndromes (MDS) with transfusion-dependent anemia requiring 4 or more red blood cell units over 8 weeks who have not responded to or have lost response to or are ineligible for erythropoiesis-stimulating agents (ESA).
IMPORTANT SAFETY INFORMATION
WARNINGS AND PRECAUTIONS
Thrombocytopenia
RYTELO® can cause thrombocytopenia based on laboratory values. In the clinical trial, new or worsening Grade 3 or 4 decreased platelets occurred in 65% of patients with MDS treated with RYTELO.
Monitor patients with thrombocytopenia for bleeding. Monitor complete blood cell counts prior to initiation of RYTELO, weekly for the first two cycles, prior to each cycle thereafter, and as clinically indicated. Administer platelet transfusions as appropriate. Delay the next cycle and resume at the same or reduced dose, or discontinue as recommended.
Neutropenia
RYTELO can cause neutropenia based on laboratory values. In the clinical trial, new or worsening Grade 3 or 4 decreased neutrophils occurred in 72% of patients with MDS treated with RYTELO.
Monitor patients with Grade 3 or 4 neutropenia for infections, including sepsis. Monitor complete blood cell counts prior to initiation of RYTELO, weekly for the first two cycles, prior to each cycle thereafter, and as clinically indicated. Administer growth factors and anti-infective therapies for treatment or prophylaxis as appropriate. Delay the next cycle and resume at the same or reduced dose, or discontinue as recommended.
Infusion-Related Reactions
RYTELO can cause infusion-related reactions. In the clinical trial, infusion-related reactions occurred in 8% of patients with MDS treated with RYTELO; Grade 3 or 4 infusion-related reactions occurred in 1.7%, including hypertensive crisis (0.8%). The most common infusion-related reaction was headache (4.2%). Infusion-related reactions usually occur during or shortly after the end of the infusion.
Premedicate patients at least 30 minutes prior to infusion with diphenhydramine and hydrocortisone as recommended and monitor patients for at least one hour following the infusion as recommended. Manage symptoms of infusion-related reactions with supportive care and infusion interruptions, decrease infusion rate, or permanently discontinue as recommended.
Embryo-Fetal Toxicity
Based on animal findings, RYTELO can cause embryo-fetal harm when administered to a pregnant woman. Advise pregnant women of the potential risk to a fetus. Advise females of reproductive potential to use effective contraception during treatment with RYTELO and for 1 week after the last dose.
ADVERSE REACTIONS
Serious adverse reactions occurred in 32% of patients who received RYTELO. Serious adverse reactions in >2% of patients included sepsis (4.2%), fracture (3.4%), cardiac failure (2.5%), and hemorrhage (2.5%). Fatal adverse reactions occurred in 0.8% of patients who received RYTELO, including sepsis (0.8%).
Most common adverse reactions (≥10% with a difference between arms of >5% compared to placebo), including laboratory abnormalities, were decreased platelets, decreased white blood cells, decreased neutrophils, increased AST, increased alkaline phosphatase, increased ALT, fatigue, prolonged partial thromboplastin time, arthralgia/myalgia, COVID-19 infections, and headache.
Please see full Prescribing Information, including Medication Guide.
You are encouraged to report adverse events related to Geron products by calling 1-855-437-6664 (1-855-GERON-MI) (US only). If you prefer, you may contact the US Food and Drug Administration (FDA) directly. Visit www.fda.gov/MedWatch or call 1-800-FDA-1088.
